Influenza Isn’t Going Anywhere
SEASONAL FLU
Only 43% of people get a seasonal flu shot. In a recent year, the CDC reported that only 56% of people who received the vaccine were protected.
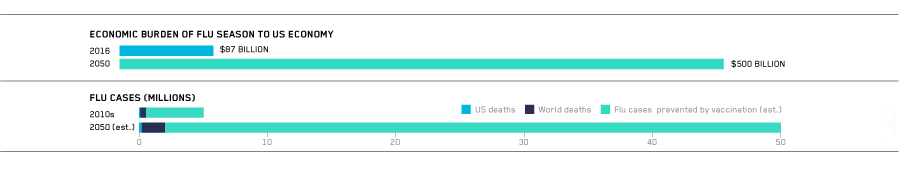
Influenza kills half a million people and seriously sickens five million more every year. Influenza was the leading cause of death in the US in 1900 and will be again by 2050 due to an aging population and vaccine ineffectiveness among the elderly.
By 2050, because of an increasingly susceptible and longer-living elderly population, the economic impact of dealing with seasonal flu alone will grow from $87 billion (2016) to $500 billion per year.
We simply need a better vaccine against influenza, one that works better and lasts longer.
Dr. Thomas Frieden
former director, CDC
A MUTATING ENEMY
Mutations in individual nucleotides accumulate in an influenza virus and lead to seasonal vaccine ineffectiveness. Influenza pandemics like those seen in 1957, 1968 and 2009—and like those to come—are due not to small, pointed mutations but instead to re-assortments of the viral genome when two or more viruses combine to create a new subtype. This commonly occurs after passing from animal to animal or animal to human.
VACCINE DEVELOPMENT
The pace of vaccine development will increase steadily as rapid sequencing technology interacts with the printing and on-demand and decentralized manufacturing of proteins. No longer will a few private companies manufacture and distribute vaccines. Instead, federal agencies will develop and send protein “blueprints” to global pharmacies for printing. This will greatly increase the pipeline speed from detection to inoculation and effectively eliminate the infrastructure problem of vaccine distribution. The problem of an individual’s choice to not vaccinate will still remain.
One day, bioelectronic, immune-like cells will be able to hunt, cut up or otherwise target viruses. They will also be programmable. Vaccines will be simple software updates. No shots needed. Today, many major disease-causing viruses are either preventable, treatable or can be managed with chronic care. Vaccine technology is less than half the battle. Access to care remains the biggest hurdle for global treatment.

THE “PENICILLIN MOMENT” IN ANTIVIRAL RESEARCH
There were almost 100 million virus-associated deaths in the 20th century. More than half of all virus-related deaths in the 20th century were due to influenza and its variants.
For a few years, penicillin was a singular “silver bullet” against bacterial diseases. In the future, a combination of surveillance and early outbreak detection, rapid vaccine development and immune system engineering could result in a post-virus world. By the end of the 21st century, viruses will still exist, and people will still die from them, but not in nearly the numbers they did in the 20th century.